Surgical Skin Cancers Management Maitland
The cause of most of the skin cancers is damage from Ultraviolet radiations emitting from the sun. The mildest form of sun damaged skin lesion is called ‘Solar Keratosis’ or a sunspot. The more invasive damage from the ultraviolet radiations create skin cancers.
There are three main types of skin cancer –
- Basal Cell Carcinoma (BCC)
- Squamous Cell Carcinoma (SCC)
- Malignant Melanoma (MM).
The BCC is the mildest and most common type of skin cancer. They are a localised cancer and do not spread through the body. BCC’s erode the site of the cancer and affect the nearby tissue. Like all skin cancers, BCCs need to be surgically removed or destroyed.
The SCC can spread elsewhere in the body if untreated. Treatment is invariably by removing the skin cancer surgically. Like the BCC, surgical removal usually means complete treatment.
The Malignant Melanoma is the worst of the three common skin cancers. If it is not removed early, it can spread to other parts of the body. Melanoma is a potentially lethal skin cancer, and the best treatment is early diagnosis and an early surgical removal before it makes its way into the bloodstream.
Some skin lesions may be difficult to diagnose accurately without a biopsy (examination under the microscope). When a lesion looks suspicious, it is usually removed surgically to ensure safety.
Elixir @ Hunter provides skin cancer checkups in Maitland Hunter Valley.
Surgical removal and defect closing methods for skin cancers
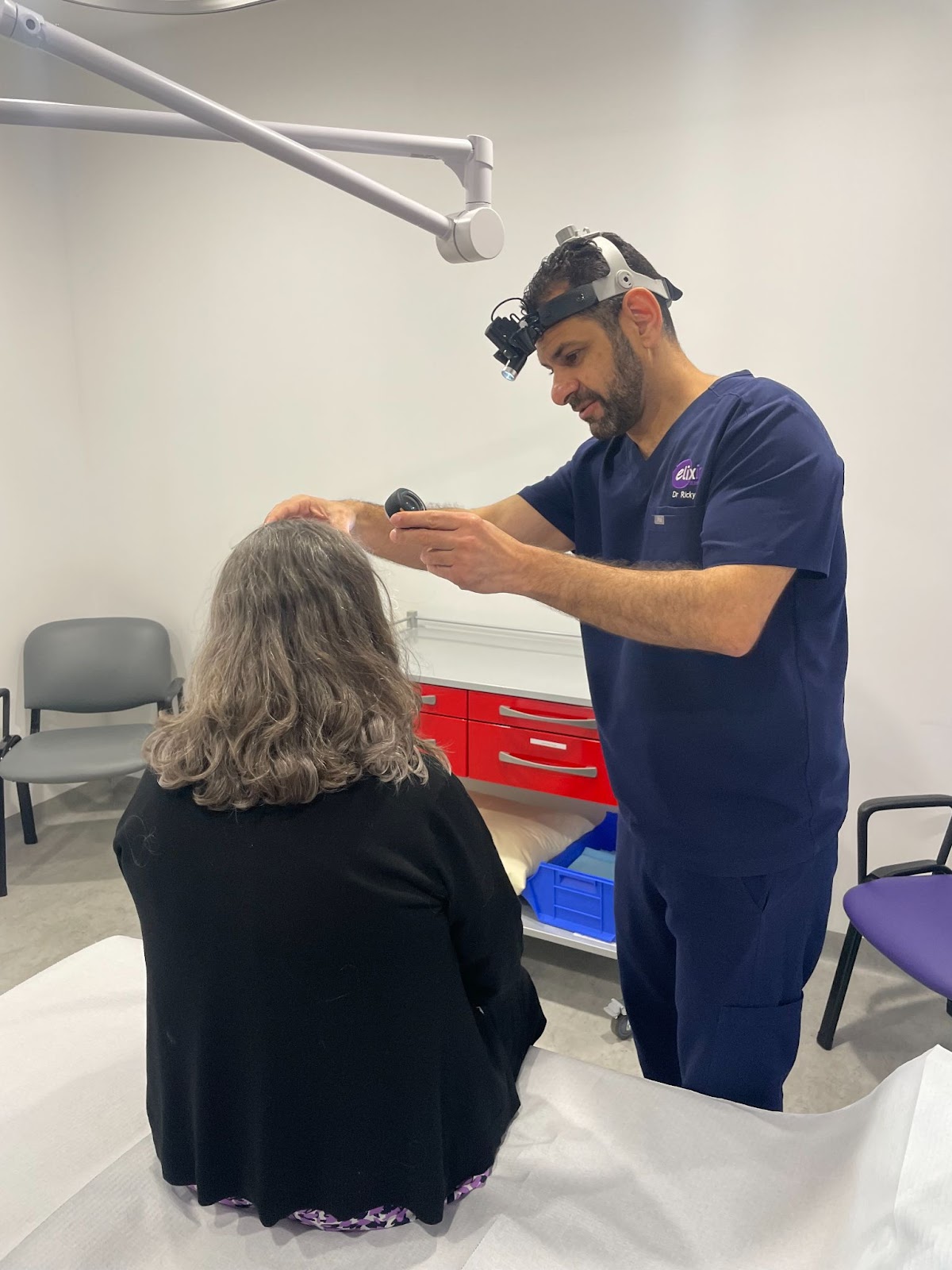
The concerning skin lesion or skin cancer is excised from the surface of the skin, right down to the base of the skin. A margin of normal skin surrounding the cancer is also removed. This safety margin is taken to minimise the chance of the lesion regrowing back. The safety margin varies depending on the type and site of the skin cancer. In the case of a melanoma, the safety margin can be quite large. Once the skin lesion or skin cancers are excised, the defect is closed either as a linear closure or with a skin graft repair or a skin flap repair.
Simple excisions and wound closure
The incision is most commonly in the shape of an ellipse. It looks like an oval with pointed ends. This type of incision makes it relatively easy to close the skin afterwards. Once the lesion is excised, the skin edges are pulled together and closed with sutures.
The excised lesion is sent to the pathologist for analysis. The pathologist will confirm the diagnosis of the lesion that was excised and they will also check the edges of the excised skin to ensure there is no skin cancer at the margins. Sometimes the cancer grows to the edge of the excision under the surface, and this is discovered only when the pathologist analyses the specimen. When this occurs, a second larger excision may be required. A scar is unavoidable whenever the skin is removed surgically, and we ensure every effort to minimise scarring.
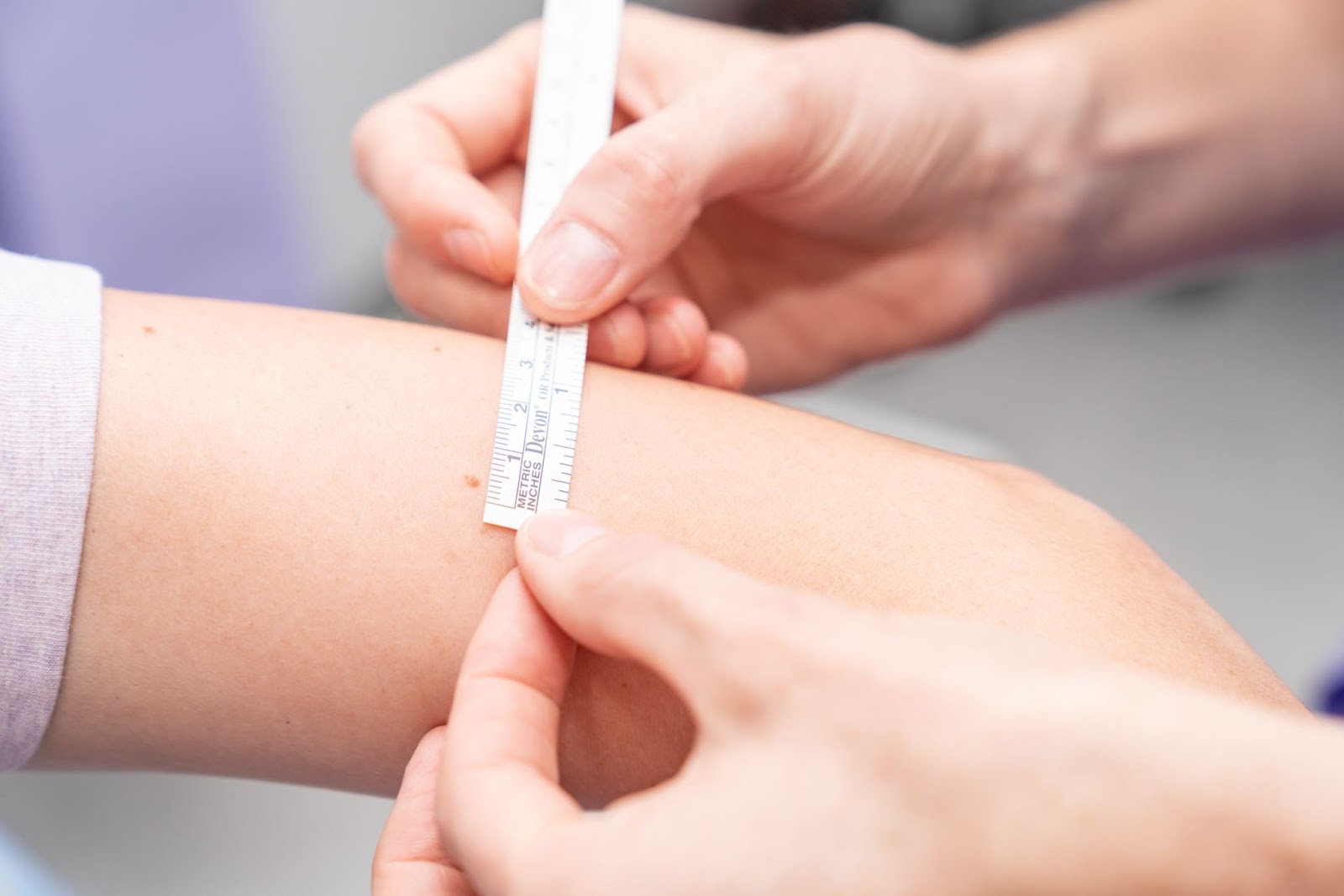
SKIN GRAFTS
When a skin lesion or ulcer is removed, the gap or defect must be closed. Most commonly skin from the edges of the incision are pulled together and stitched as a simple or linear closure. Sometimes this is not possible as the gap might be too large. Alternatively, pulling the skin edges together might place too much strain on this skin.
In this situation, a skin graft may be used. This involves taking skin from somewhere else on the body and attaching (or grafting) this skin to the gap. In this way, extra skin is available to fill the gap without placing too much tension on the surrounding skin.
The place where extra skin is obtained from is called the “donor site”. Where this skin goes is called the “graft site”. A full thickness skin graft is where all layers of skin are grafted into the gap. The donor site may be taken from any part of the body. The skin in different parts of the body has different colours and different texture. A full thickness graft may or may not grow hair in its new home and may look quite different to the surrounding skin.
The first step is to remove the mole, skin cancer or ulcer in the usual manner under the effect of local anaesthetic. Once removed, this lesion is sent to the Pathology where it is analysed. The pathology results of usually takes around a week finalise.
Once the specimen has been removed and if the defect needs a skin graft, a suitable donor site is identified, and a local anaesthetic is administered. A scalpel is commonly used to excise the section of skin from the donor site. The defect left after the graft has been removed needs to be closed, and most commonly this site is directly sutured.
Once the donor skin is prepared, it is sutured in place. Then a dressing is placed over the graft. It is then a matter of waiting for skin graft to heal in its new home. When this happens, the graft is said to have been “taken”.
Sometimes the graft fails to “take”. This is not common and is likely to be related to poor circulation to the site or if the site becomes infected. The greatest healing risk is present when the graft site is below the knee. Areas on the shin and foot are often poor at healing.
The patient will end up with two scars. There is the donor site scar as well as graft scar. The graft needs good care after the operation. Knocking or bumping the graft site can upset the graft, and in these cases, the graft can take up to several months to completely heal.
Skin Flap Repairs
A skin flap repair is another way of closing the defect after removal of the skin cancer when a simple linear closure of the gap or defect is not possible.
This involves repositioning skin from the surrounding area and suturing the skin in the gap to be closed. Skin flaps are often used when skin is tight at the site of the lesion, but skin nearby is looser. Moving nearby skin into position means that larger and more complicated skin incisions are required. This means there will be more sutures and a larger scar. Whenever the scar is larger, there is a greater risk of the result being unsightly. Every effort is made during the procedure to make the wound as acceptable as possible.
The procedure involves excision of the skin cancer or ulcer in the usual manner under the effect of local anaesthetic. Once removed, this lesion is sent to the Pathology Department where it is analysed. A report on the lesion usually takes around one week. Immediately after the lesion is removed, further skin incisions are made into nearby skin. A piece of skin is then raised from one site and moved to a nearby location. During a flap repair, a part of the skin always remains connected to adjacent skin. This connection is called the base of the flap. The flap gets its blood supply through the base of the flap. Then the flap is sutured in place.
There are a number of types of skin flaps. The differences are in the way that incisions are made, and the way that the flap is pushed into place. The decision on the type of flap is based on the location of the lesion and the nature of the skin surrounding the lesion. Flap surgery usually results in a zig zag type of scar, or two scars running parallel, or a scar that turns corners. Your doctor will explain about the type of flap needed for your procedure.
There are some possible complications that can occur after a flap surgery. Occasionally, the ends of the skin flap fail to survive the move. It is more likely if the patient’s circulation is poor. It is also more likely if the area gets infected. Older patients with flaps heals less well than younger patients.
When this happens, the edge of the flap usually heals slowly and with a larger scar. Contractures can occur where the flap is placed. This can produce a tightness in the skin and sometimes needs further surgical attention. This problem is usually only associated with large skin flaps, or flaps in awkward sites. Every effort is made during the procedure to allow the wound to heal with a minimum of scarring. Looking after the wound also helps minimise the scarring.
