Did you know Melanoma can become life-threatening in as little as 6 weeks?
The three common types of skin cancers are:
- Squamous Cell Carcinoma or SCC
- Basal Cell Carcinoma or BCC
- Malignant Melanoma or MM
Melanoma is the most dangerous amongst the common types of skin cancers. It usually starts as a simple skin lesion. The cancer cells then get into the bloodstream and can spread to any other part of the body. It is the spread elsewhere that can result in death. Oot of every ten people that die of skin cancer, eight die of melanoma.
Elixir @ Hunter is skin cancer clinic in Maitland, offering quality skin cancer treatment. Book your consultation today!
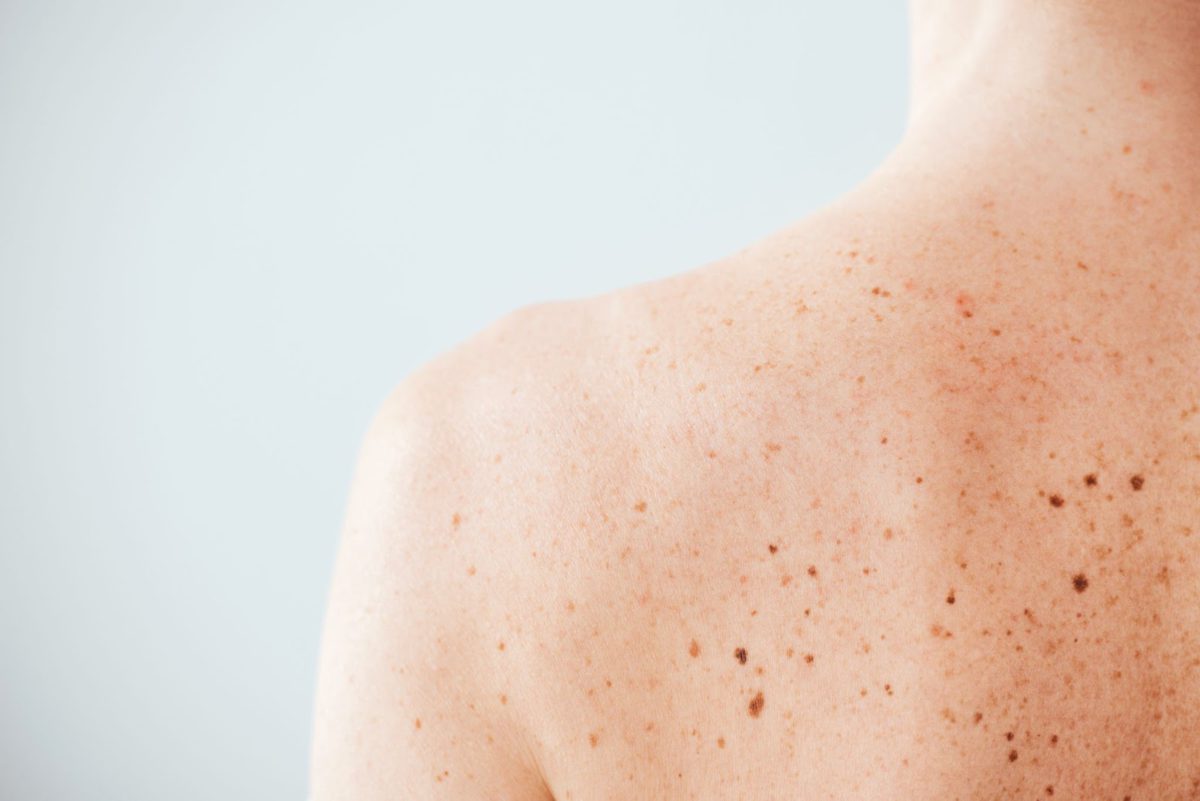
What does it look like?
It is generally a dark coloured mole that may have an irregular shape. Most of these lesions are flat lesions within the skin rather than sticking out from the skin. Most of them will appear just like a common flat mole with asymmetrical distribution of pigmentation but they are usually asymptomatic.
Most of these lesions are neither painful nor itchy, and most can’t be felt. Some melanomas can appear as a bump in the skin. A melanoma that can be felt is more serious than one that can be seen but not felt.
Most of the melanoma grows horizontally on the skin surface before they start going deeper. The depth of the melanoma is the most important prognostic criteria. Melanoma over 0.75 mm Breslow thickness (measuring scale for melanoma) can have more potential to spread in the body as compared to thinner melanomas. The melanoma that appears as a bump in the skin has more potential to spread as this type of melanoma starts to grow vertically almost from day 1, and these are the melanomas which can become life-threatening in as little as 6 weeks.
Risk Factors
The most common site for melanoma is on the arms, legs or back, but they can grow on any area of the skin including palms, soles and under the nails.
Around 90% of the melanomas are linked to damage from Ultraviolet or UV rays.
A genetic condition called “Dysplastic Naevus Syndrome” or “Atypical Naevus Syndrome” is a major risk factor for melanoma. Multiple dysplastic melanocytic naevus syndrome (MDMNS) is a condition where a patient has 5 or more dysplastic melanocytic naevi (DMNs). These people are at substantial risk of developing melanoma. MDMNS patients have a future melanoma risk more than 40 times the risk of other patients.
Dysplastic moles mostly look like very dark or black moles. They often have a strange irregular shape, like the map of a country, but are otherwise smooth to touch.
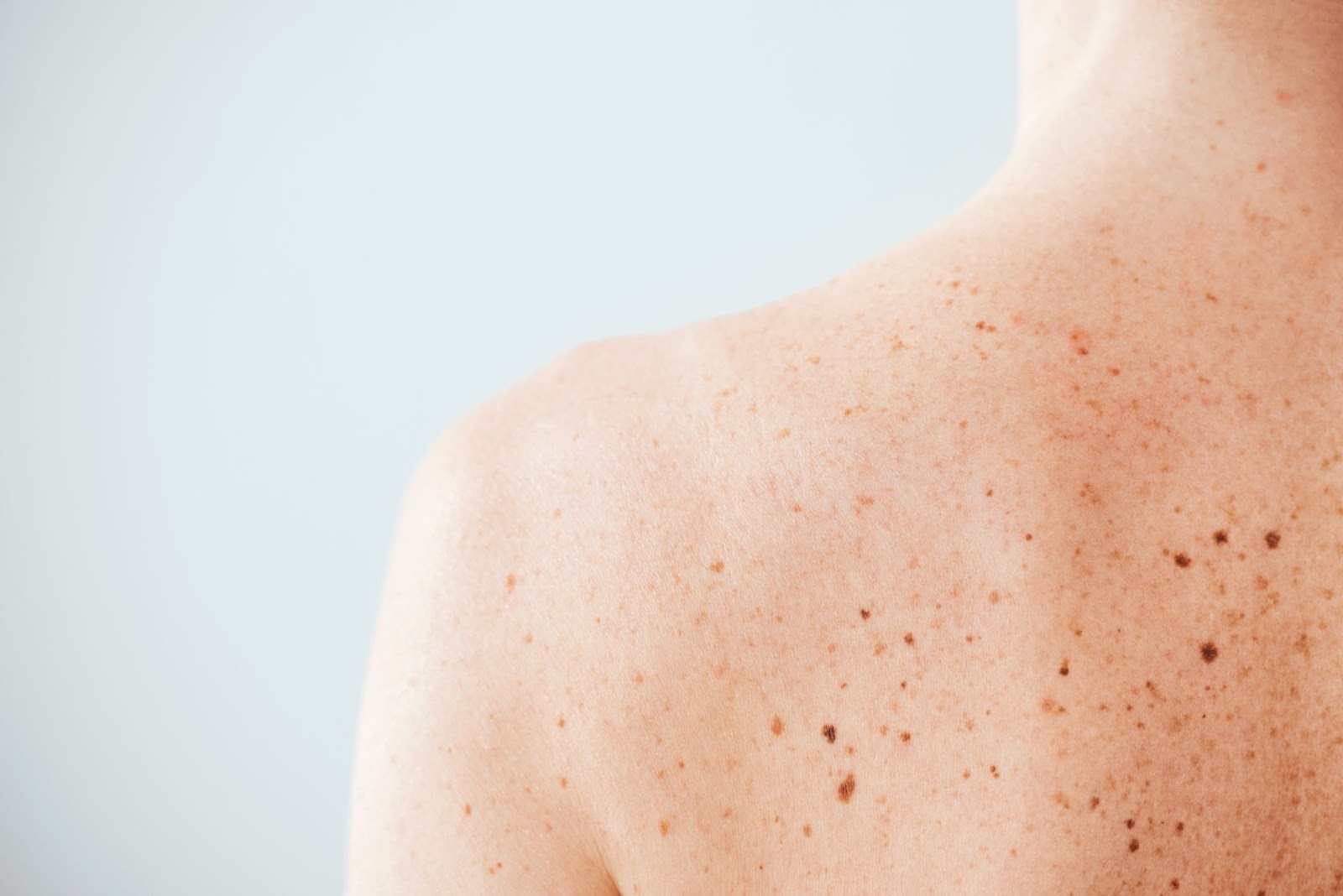
Patients with MDMNS are at high risk of melanoma. It is therefore essential that extreme measures are taken to avoid sun damage.
Regular careful skin checks are essential and are the key to MDMNS. In most of these people, melanoma mostly grows from normal looking skin rather than from existing dysplastic moles. As such, simply removing lots of dysplastic moles is not the answer.
These patients need a regular 6 monthly professional skin checkup and they also need to check their own skin every 2-3 months or even every month. There are parts of your skin you can’t see. Ask your partner or friend to check these areas for you. If any new or changing mole develops between the scheduled appointments, do not wait. Please make an appointment to see your doctor as soon as possible.

Where can melanoma spread into the body?
Melanoma can spread anywhere. The commonest site is lymph nodes. It can also spread to nearby skin sites. It is more serious when it spreads to places like the lungs, liver and brain. A spread to these distant sites has a concerning risk of death.
What is the usual treatment?
Skin melanoma lesions are invariably excised. Melanoma treatment is almost always in at least two stages.
The doctor will initially take out just the lesion with a narrow margin to confirm the diagnosis and to check the depth and other prognostic factors of the melanoma.
Once the diagnosis and other prognostic factors are confirmed, a wider excision is organised. This second excision requires a wide ring of non-involved skin being removed from around the melanoma. The clearance is usually 1 or 2 cm of apparently normal skin on all sides.
Early diagnosis and treatment of a melanoma is the key to maximising survival. Try to catch the melanoma before it has spread.
Can the melanoma come back?
Wide excision with the recommended melanoma margin guidelines minimises the risk of recurrence of melanoma.
The chances of recurrence of melanoma depends on individual factors including: the thickness the cancer penetrates the skin, its body location, whether the cancer had an ulcer on its surface, whether there are lymph nodes involved and whether it is spread to other places in the body.
What happens if a melanoma spreads in the body?
While usually fatal in the past, there are now new treatments available for metastatic melanoma. If you have a metastatic melanoma, you will be referred to a medical oncologist, a specialist in these cancer drug therapies.
If the melanoma has spread to a single site, surgery can be helpful.
Radiation is not commonly used for managing melanoma, but it can be useful when a site of spread produces marked local pain.
Risk of getting more melanomas after a diagnosis of melanoma
Any person who has developed a melanoma is susceptible to further skin cancers. This includes a further lifetime risk of getting melanoma and non-melanoma skin cancers.
It is recommended to have regular and ongoing skin checks for life.
How to reduce the risk of getting a melanoma?
- Reducing sun exposure helps. Suntan or sunburn means future skin cancer risk. Avoid outdoors 11:30 AM to 3:00 PM.
- Apply and reapply sunscreen regularly.
- Shade over the pool & playgrounds protects our kids.
- Long-sleeved shirts.
- Hats with a brim.
- Drive with windows up.
- Sunglasses.
- Long pants or skirts.
- 50+ Sunscreen.
- Umbrellas and shelters.
- Enclosed tractors.
- Check your own skin each month.
- See your doctor if any new or changing skin lesion develops.
- Have a regular skin checkup with a professional every 1-2 years.
- Patients who have had a melanoma need 6 monthly skin checks by a doctor for life.
If you need skin cancer treatment in Newcastle or Maitland then call us today and book a consultation. Our coverage area: Newcastle, Singleton, Rutherford, Branxton, Cessnock, Aberglasslyn, Lochinvar
