Psoriasis
What is Psoriasis?
Psoriasis is a chronic, immune-mediated inflammatory skin condition characterised by red, thickened plaques with overlying scale. It occurs due to accelerated skin cell turnover, where skin cells renew in days rather than weeks, leading to inflammation, scaling, and visible skin changes.
Psoriasis affects approximately 2–4% of the population. It is not contagious, but its chronic and visible nature can significantly affect physical comfort, emotional wellbeing, and quality of life. While psoriasis cannot currently be cured, symptoms can often be effectively controlled with appropriate, ongoing management.
Understanding Psoriasis
Psoriasis can occur at any age, with common peaks in early adulthood and later life. A genetic predisposition plays an important role, and around one-third of affected individuals have a family history of the condition.
The immune system is central to psoriasis development, and symptoms may fluctuate over time with periods of flare and remission.
Who Gets Psoriasis?
- Psoriasis can occur at any age but typically peaks between 15–25 years and 50–60 years.
- It is more common in Caucasians but can affect people of any ethnicity.
- One-third of individuals with psoriasis have a family history of the condition.
What Causes Psoriasis?
Psoriasis is an immune-mediated genetic skin disease, involving an interaction between the immune system and genetic predisposition. Certain triggers may worsen psoriasis, including:
- Infections (e.g., strep throat)
- Skin injuries (cuts, burns, or sunburn)
- Stress and emotional events
- Cold, dry weather
- Obesity, smoking, or alcohol consumption
- Certain medications (e.g., beta-blockers, lithium)
What Does Psoriasis Look Like?
- Red, scaly plaques with clearly defined edges.
- Silvery white scaling, except in skin folds where plaques appear shiny or moist.
- Common sites include the scalp, elbows, knees, and lower back.
- Symptoms may include itching, skin cracking, or painful fissures, especially on the palms and soles.
- Psoriasis can result in post-inflammatory pigmentation changes (dark or pale marks) that fade over time.
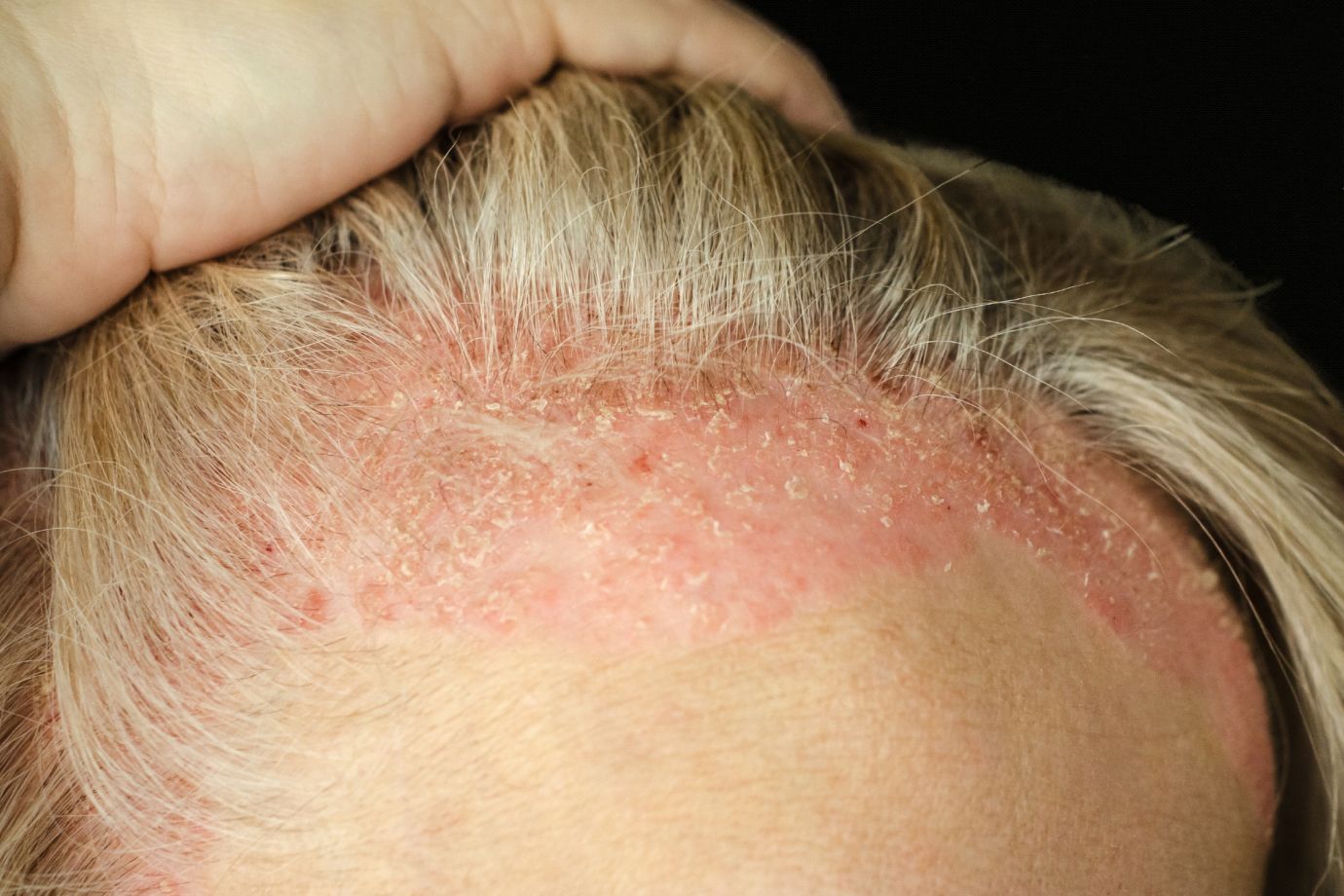
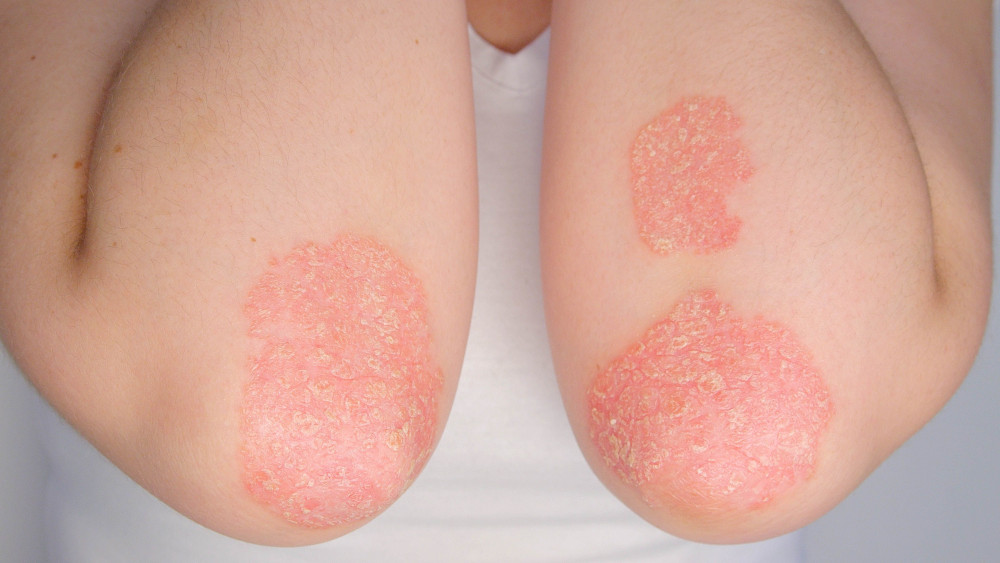
Common Features of Psoriasis
Psoriasis may present as:
- Red, well-defined plaques with surface scale
- Silvery-white scaling (or smooth, shiny plaques in skin folds)
- Itch, skin tightness, cracking, or discomfort
- Post-inflammatory pigmentation changes after plaques resolve
Commonly affected areas include the scalp, elbows, knees, lower back, palms, and soles, though psoriasis can occur anywhere on the body.
Triggers That May Worsen Psoriasis
While triggers vary between individuals, flare-ups may be associated with:
- Infections (such as streptococcal throat infection)
- Skin injury or sunburn
- Psychological stress
- Cold or dry weather
- Smoking, alcohol use, or excess weight
- Certain medications
Identifying and managing triggers is an important part of long-term control.
Treatment Approach
Psoriasis management is individualised and depends on disease severity, extent, location, and response to previous treatment. Options may include topical therapy, phototherapy, or systemic treatments.
Phototherapy for Psoriasis

Phototherapy is a cornerstone treatment for moderate to severe psoriasis and for widespread or treatment-resistant disease.
Narrowband UVB (nbUVB) phototherapy is the most commonly used and well-established form. It involves exposing affected skin to carefully controlled ultraviolet light under medical supervision.
Phototherapy may help:
- Reduce skin inflammation
- Slow excessive skin cell turnover
- Decrease scaling and plaque thickness
- Improve symptom control and remission duration
Treatment is delivered using medical-grade equipment in a clinical setting. Sessions are brief and scheduled over a treatment course to balance effectiveness and safety. For selected cases, other light-based options such as excimer laser or PUVA may be considered.

Other Treatment Options
Depending on severity and response, management may also include:
- Topical treatments: emollients, vitamin D analogues, corticosteroids, keratolytics
- Systemic medications: for more extensive disease
- Biological therapies: for severe psoriasis or associated joint involvement
Your clinician will discuss appropriate options during consultation.
Frequently Asked Questions
Is psoriasis contagious?
No. Psoriasis cannot be passed from person to person.
Who is suitable for phototherapy?
Phototherapy may be recommended for individuals with moderate to severe psoriasis, widespread disease, or psoriasis that has not responded adequately to topical treatment. Suitability is assessed during consultation.
Is phototherapy safe?
When delivered under medical supervision, narrowband UVB phototherapy is generally well tolerated. Potential risks and expected outcomes are discussed prior to treatment.
How long does phototherapy take to work?
Many patients notice improvement after several weeks of regular treatment. Response varies between individuals.
Can psoriasis be cured?
There is currently no cure. Treatment focuses on controlling symptoms, reducing flare-ups, and maintaining skin health over time.
Long-Term Psoriasis Management
Psoriasis is a long-term condition that benefits from ongoing care and regular review. Effective management may include:
- Education about the condition and treatment options
- Identification of individual triggers
- Tailored treatment plans, including phototherapy when appropriate
- Ongoing monitoring and adjustment of therapy
Book a Consultation
If psoriasis is affecting your comfort, confidence, or quality of life, professional assessment is the first step. A consultation with a qualified medical practitioner allows for accurate diagnosis and discussion of personalised treatment options, including medically supervised phototherapy.
Book an appointment to explore evidence-based care designed to help you manage psoriasis with confidence.
